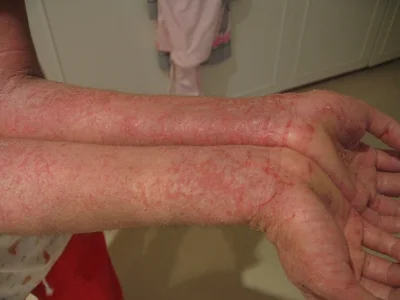
Epidermolysis bullosa (EB) is a terrible hereditary disease that results in blistering skin and can become so severe that the skin falls off the body (I highly recommend that you do not search for images of the disease, really). Severity levels vary but this disease can be lethal and the age of death is often very young. While recently many stem cell research advancements have been made bringing new treatments to young patients, treatments for the disease are lacking and a full understanding of the disease is not complete.
EB is a disease that is characterized by antibodies that target type VII collagen (COL7), an important part of the skin. In previous experiments, when mice are immunized for COL7, skin blisters result in 80% of the mice however 20% of mice remain healthy. To look at why this happened, scientists in Germany looked at the innate and adaptive immune response of mice that were healthy and compared this to the mice that became sick after immunization and published the results in the Journal of Autoimmunity.
They studied the skin microbiome of the mice by taking a biopsy prior to immunization because the skin microbiome has been shown to influence cutaneous inflammation. One of the major findings was that in the mice that did not develop the clinical symptoms of EB, there was greater richness and diversity of the skin microbiome before immunization. This showed that the results of the experiment could have been predicted prior to experimentation and therefore is an important factor in future studies looking at the transition from autoimmunity to the onset of autoimmune disease.
These results also lead us to the conclusion that it may be possible to prevent or reduce clinical inflammation in autoimmune disease by influencing the skin microbiome.